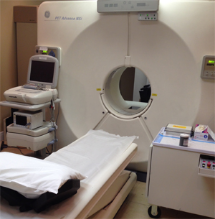
Oncology Imaging
Positron Emission Tomography (PET) has become an essential diagnostic tool physicians use to reveal the presence and severity of cancers. PET imaging helps physicians detect cancer, evaluate the extent of disease, select the most appropriate treatments, determine if the therapy is working, and detect any recurrent tumors.
Before a PET scan, the patient receives an intravenous injection of radioactive glucose. Many cancer cells are highly metabolic and rapidly synthesize the radioactive glucose. Information regarding the location of abnormal levels of radioactive glucose obtained from the whole-body PET scan helps physicians effectively pinpoint the source of cancer and detect whether cancer is isolated to one specific area or has spread to other organs.
From this information physicians can plan an effective treatment strategy. Treatment options include surgery, radiation therapy, systemic therapy, or a combination therapy where one or more of these options are combined.
During the course of treatment, the information from the PET scan allows physicians to monitor the effectiveness of cancer therapies and provides physicians with the opportunity to change the treatment strategy if it is not working, avoiding the cost and discomfort of ineffective therapeutic procedures.
After completing the treatment regimen, a follow-up whole-body PET scan can provide information to assess if the treatment was successful and if areas that were previously abnormally metabolically active have responded. Often, scar tissue at the site of surgical resection or radiation treatment may appear as an abnormality on the CT scan. The PET scan can detect residual disease within the scar tissue and indicate if the treatment was successful or if the tumor has returned.
PET scans provide information to help physicians:
- Locate the site of the cancer
- Determine the size of the tumor
- Differentiate benign from malignant growths
- Discover if the cancer has spread
- Select treatments that are likely to be appropriate
- Monitor the success of therapy
- Detect any recurrent tumors